WHAT IS DEEP VEIN THROMBOSIS (DVT)?
Legs have two sets of veins—superficial veins and the deep veins that drain blood from the leg muscles. A deep vein thrombosis (DVT) is a blood clot that forms in the veins deep in the leg, usually in the calf or thigh, although DVT can occur in other veins including the pelvis and rarely in the arms [1, 2]. DVT can partially or completely block blood flow through a vein but not everyone with DVT will experience symptoms [2].
Doctors refer to DVT as distal or proximal; distal DVT refers to DVT of the calf, proximal DVT refers to DVT above the knee and above a major vein called the popliteal vein [3]. Most DVT form in the calf area and many do not cause any symptoms. Proximal DVT is more serious than distal DVT. One in two people with untreated proximal DVT will develop symptomatic PE within 3 months [3].
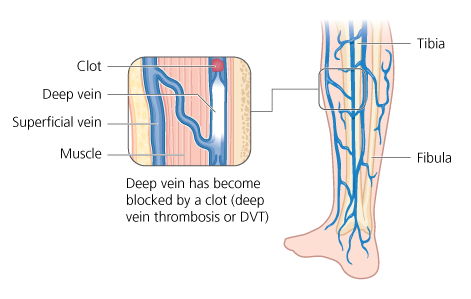
The figure shows a typical DVT in a deep vein of the leg.
SYMPTOMS OF DVT
In many cases of DVT, the clots are small and do not cause any symptoms [3]. Most patients have symptoms when there is proximal vein involvement and these symptoms can include [2]:
- Swelling—this is usually different from the mild ankle swelling that many people get during long haul flights and the entire leg can swell
- Pain or tenderness of the leg that is noticeable or may be worse when standing or walking
- Discolouration of the leg, which can appear a blue or red
- A feeling of increased warmth in the leg
Always talk to your doctor if you have any concerns about DVT or if you think you have symptoms of DVT.
IS DVT COMMON?
Each year, about 160 out of 100,000 people are affected by DVT [4], and venous thromboembolism is one of the leading causes of preventable death in Australia, accounting for almost 10% of all hospital deaths [7]. DVT became well known several years ago because of its association with flying for long periods (often called ‘traveller’s thrombosis’ or ‘economy class syndrome’), but the risk of getting a DVT is higher in hospitalised patients. Only about one in 6000 people who go on a long flight (more than 4 hours) will develop DVT [5], but if you are in hospital particularly for a major operation or because of a serious illness, your risk of having a blood clot in your leg or lungs is much higher than usual [1]. Hospitalised patients are over 100 times more likely to develop a DVT or PE compared with the rest of the community [6].
COMPLICATIONS OF DVT
A DVT may not cause further problems, but complications of DVT can occur. These include:
- Pulmonary embolism (PE)—when part of the clot breaks off and blocks blood flow to a lung [1]
- Recurrence—despite treatment, DVT can recur [3]
- Post-thrombotic syndrome—characterised by pooling of blood, chronic leg swelling, pain, discoloration of the skin, and leg ulcers [2]; about 10% of cases with symptomatic DVT will suffer severe post-thrombotic syndrome within 5 years [3]
This website offers general information only. Please see a healthcare professional for medical advice.
REFERENCES
- National Blood Clot Alliance. At-a-glance: blood clots. Accessed on 15 April 2025.
- Cleveland Clinic. Deep Vein Thrombosis (DVT). Accessed on 15 April 2025.
- Ho WK. Deep vein thrombosis. Australian Family Physician 2010; 39:468-74.
- The Australia and New Zealand Working Party on the Management and Prevention of Venous Thromboembolism. Prevention of venous thromboembolism (5th Edition). 2010.
- World Health Organisation. 2007. Who Research Into Global Hazards of Travel (WRIGHT) Project, Final Report of Phase I. Accessed on 15 April 2025.
- Khalafallah AA et al. Venous thromboembolism in medical patients during hospitalisation and 3 months after hospitalisation: a prospective observational study. BMJ Open 2016; 6(8): e012346.
- Australian Commission on Safety & Quality in Health Care - Venous Thromboembolism Fact Sheet
